What the May 2026 NDIS Budget Really Means for Small Providers
The May 2026 federal budget drops on 12 May. But the government has already signalled what is coming. This is Article 2 of a 5-part series on NDIS productivity, written by an active Support Coordinator who works with the system every week.
This article publishes before the 2026-27 federal budget on 12 May. The government has already made a series of pre-budget announcements that tell us, with reasonable certainty, where the NDIS is heading. If you are waiting for budget night to start preparing, you are already behind. Here is what has been signalled, what it means for small providers, and what you can do about it right now.
The May 2026 federal budget lands on 12 May. The pre-budget announcements already tell small NDIS providers what to expect.
It is Sunday evening. You have been reading the NDIS coverage all week.
Participant budgets are being reset. Support coordination is moving to a commissioned model. Unregistered providers face new registration requirements. The headlines are loud and the details are thin.
If you run a small NDIS practice, a sole trader operation, or an allied health service with NDIS participants, you are probably asking one question: what does any of this actually mean for my practice on Monday morning?
This article strips out the political noise and focuses on what has been confirmed, what it means for small providers specifically, and what the ethical operators in this sector should be doing right now, before the budget even lands.
What Has the Government Actually Confirmed Before the Budget?
Several significant changes have already been announced as pre-budget signals. These are not speculation. They are confirmed government policy positions that will be legislated through the National Disability Insurance Scheme Amendment (Securing the NDIS for Future Generations) Bill, which is set to be introduced following the budget release.
The four confirmed changes that matter most for small providers:
Participant budget reductions: Average participant budgets for social, civic and community participation supports are expected to drop from around $31,000 to $26,000 progressively from 1 October 2026, returning to approximately 2023 levels.
Support coordination commissioning: The government will move to a commissioned model, selecting support coordinators and plan managers from a government-vetted list. The stated aim is to reduce spending in this area by 30 per cent.
Mandatory registration expansion: From 1 July 2026, mandatory registration begins for Supported Independent Living and platform providers. Broader mandatory registration for providers delivering personal care and daily living supports rolls out from July 2027 through to end of 2030.
Plan reassessment restrictions: Unscheduled plan reassessments will be restricted to exceptional circumstances only. Currently one in five plans is reassessed each year, with an average 20 per cent plan increase as a result. That pathway closes.
Why Are Participant Budgets Being Cut and What Does It Mean for Providers?
The NDIS has a public image problem. Between the ABC News explainer (21 April 2026) and the Disability Royal Commission fallout, the media framing often suggests a sector "out of control."
Government rhetoric has hardened accordingly. With the NDIS Sustainability Taskforce charged with cutting annual spending growth from 10% down to between 5% and 6%, the language of reform is increasingly the language of restriction.
Here is the part that stings: Most of the "shonky operator" commentary does not apply to you. You are not billing ghost hours or rorting plans. But the regulatory response does not differentiate. When the Commission tightens registration rules, it tightens them on everyone.
Why is the May 2026 Federal Budget a Tipping Point for NDIS Providers?
The social and community participation category has been the fastest-growing area of NDIS expenditure. Over five years, spending in this category tripled from approximately $4 billion to $12 billion annually. The government has stated this level of growth is unsustainable.
From 1 October 2026, budgets for social, civic and community participation supports and capacity building daily activities will be progressively adjusted. The government has confirmed essential core supports including personal care, daily living, disability accommodation and transport are protected.
What this means for small providers:
Providers whose service mix is weighted toward community participation activities face a direct revenue reduction as participant budgets in this category shrink. The adjustment is not optional and it is not negotiable.
The providers best placed to absorb this change are those who have already diversified their service mix toward core supports, those whose documentation and compliance systems are strong enough to withstand tighter auditing, and those whose operational costs are lean enough to remain viable at lower billing volumes.
Providers who have been running manual administration systems, loose documentation habits, and high overhead relative to billing volume will feel this first.
The ethical note: The cuts are targeted at excess and fraud, not at quality providers. But the regulatory response does not differentiate between good operators and poor ones. Tighter rules tighten on everyone equally.
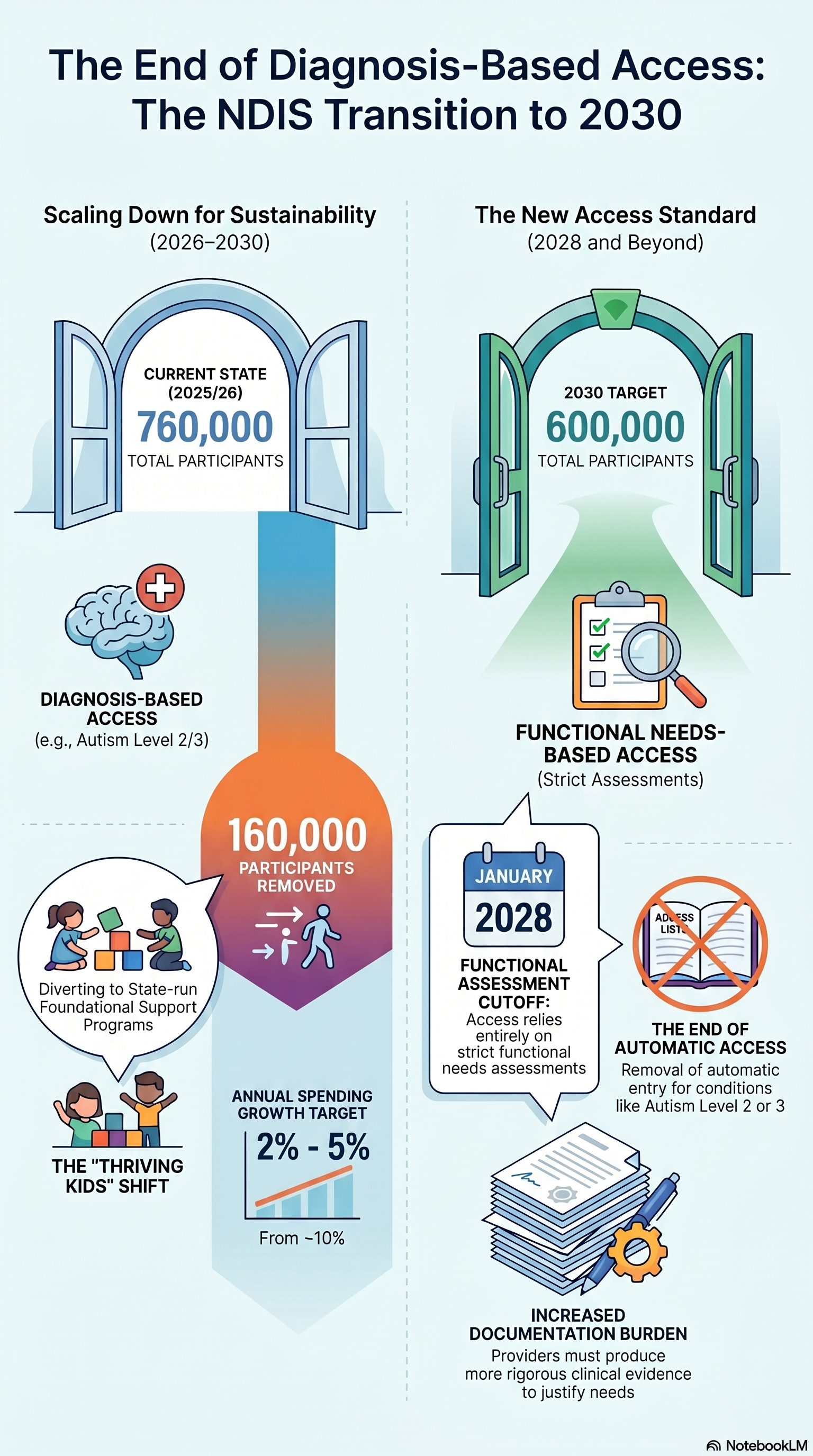
From 760,000 participants today to a 2030 target of 600,000. The transition to functional needs-based access increases the documentation burden on every provider still in the scheme.
What Does the Support Coordination Commissioning Model Mean in Practice?
This is the announcement that has generated the most anxiety among support coordinators. It deserves a clear explanation rather than alarm.
The government has confirmed it will commission a panel of plan management providers and a new support coordination function. Participants will still have choice, but within a government-vetted approved list. The new plan management commissioning model begins from 1 October 2027 with a six-month transition period. The new support coordination function follows from 1 July 2028.
This is not happening immediately. But the direction is clear and the timeline is set.
What this means for support coordinators right now:
The providers who will make it onto the commissioned panel are those who can demonstrate quality, integrity and compliance with evidence. Not those who have been operating informally, with paper-based systems, and unverifiable outcomes.
If you are a support coordinator or support coordination organisation and you cannot currently produce clean documentation of your practice quality, your participant outcomes and your compliance record, the next twelve months are your preparation window. Not your grace period. Your preparation window.
The government has stated the aim of the commissioned model is to reduce spending in this area by 30 per cent. Some providers will not be on the panel. The ones who are will be those who built their practice on evidence, not assumption.
Why Is Mandatory Provider Registration Expanding and Who Does It Affect?
One of the consistent themes across the NDIS reform announcements is provider quality and fraud prevention. The government has highlighted significant problems with fake claims, low-quality services and organised exploitation of the scheme.
The response is mandatory registration expansion. From 1 July 2026, mandatory registration begins for Supported Independent Living providers and platform providers. From July 2027, registration requirements broaden to providers delivering personal care and daily living supports, rolling out through to end of 2030.
A new enrolment system with a minimum basic level of identifiable information on most NDIS providers is also being introduced.
What this means for unregistered providers:
If you are currently operating as an unregistered provider, the window of operating outside the registration framework is closing. The timeline gives you runway, but it is a defined runway with a known end point.
Registration requires documented quality systems, staff compliance records, incident management processes and audit readiness. Providers who build these systems now are building an asset. Providers who wait until registration becomes mandatory are building them under pressure.
The practical upside for registered providers:
The crackdown on unregistered providers is good news for ethical registered operators. The providers currently undercutting the market by operating without registration costs will face a choice: register and meet the standard, or exit the scheme. For providers doing the work properly, this levels the playing field.
Mandatory registration expands from July 2026. Providers who build compliant systems now are building an asset, not meeting a deadline.
What Should Small Providers Actually Do Before 12 May?
The budget lands on 12 May. Between now and then, the pre-announced changes give you enough certainty to act. Here is what the ethical operators in this sector should be doing right now.
Audit your service mix:
Look at what proportion of your current billing comes from social and community participation supports. If it is significant, model what a reduction to 2023 budget levels looks like for your revenue. Plan the gap before it arrives.
Review your documentation systems:
The commissioned support coordination model will favour providers with clean, verifiable documentation of practice quality and participant outcomes. If your case notes, service agreements and incident records are not audit-ready today, start there.
Check your registration status:
If you are unregistered and delivering supports that fall within the expanding mandatory registration categories, understand your timeline and start the registration process. Do not wait for the legislation to pass.
Reduce your administrative overhead:
The providers who survive margin compression are those who spend the least time on administration relative to their billable hours. Every hour spent on manual documentation, compliance spreadsheets and chasing paperwork is an hour not delivering services or an hour of unpaid overhead. This is the productivity argument in practical terms.
Build your compliance evidence base:
The new enrolment system will require identifiable information on providers. The commissioned model will require demonstrated quality. Both require that your systems are producing evidence, not just activity.
What Will This Series Cover Next?
This is Article 2 of the NDIS Productivity Series. The full series:
Article 1: The Ethical Operator's Dilemma: Why NDIS Productivity Matters More Than Ever in 2026. [Read here]
Article 2: What the May 2026 NDIS Budget Really Means for Small Providers. You are reading it.
Article 3: The Productivity Paradox: Why Doing More Manually Is Hurting Participant Care. Coming soon.
Article 4: 7 Practical Productivity Wins for NDIS Providers in 2026. Coming soon.
Article 5: AI and NDIS Documentation: What Is Safe, What Is Risky, and What Actually Works. Coming soon.
Need Help Getting Your Practice Budget-Ready?
If the pre-budget announcements have raised questions about where your practice stands, here is where to start.
👉 [Book a free 30-minute consultation] : No sales pitch. A conversation between practitioners about what your practice needs to address the future direction the NDIS is heading towards.
👉 [Learn how MedPrivacy protects your practice]: If you are using AI for documentation, make sure you are doing it safely and compliantly.
--—————————-
Sinclair Hurtis is an active NDIS Support Coordinator (partnering with My Ability Services in Melbourne) and the founder of CollabEdge Solutions. He builds practical tools for ethical NDIS providers, starting with the problems he encounters in his own experiences